Itchy legs are a lesser-known symptom of varicose veins but this irritating complication will often send patients rushing to their doctor.
If you’re wondering why are varicose veins itchy, it’s due to a condition called Varicose Eczema, or Stasis Dermatitis, which can develop in some patients suffering from vein disease.
How does Varicose Eczema develop?
To understand this, let’s first look at what causes varicose veins in the first place. When vein valves or vein walls become damaged, blood starts slipping backwards instead of flowing toward the heart. As a result, circulation through that area slows and your skin doesn’t get all the oxygen and nutrients it needs to stay healthy.
Malfunctioning valves and – subsequently – varicose veins and varicose eczema can happen for many reasons (see: varicose vein causes), with the most common being age, family history, and hormonal changes.
It’s important to note that varicose eczema may lead to a venous ulcer, so it’s important to treat it early.
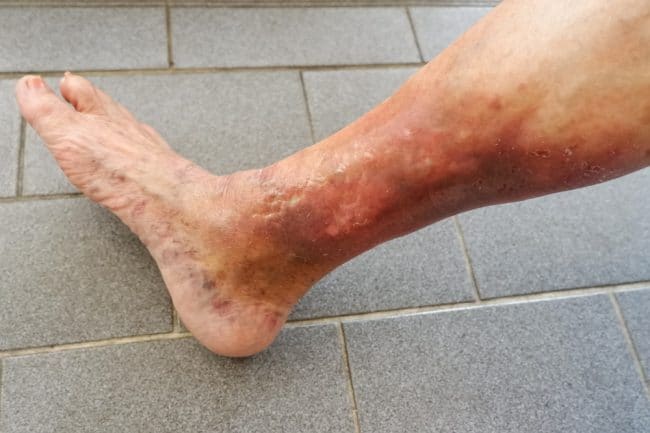
How to treat itchy varicose veins
Varicose eczema, also called venous eczema, can be treated in a number of ways. Here are a few tips:
- Moisturise: Apply at least twice a day to calm the irritated skin. It’s recommended to try something with a thick consistency, which is natural and free from perfumes.
- Avoid scratching: It sounds counterproductive but scratching the itchy areas can often worsen the itch. Scratching can lead to further trauma in the vein and more histamine produced by the body. Scratching can also cause cuts that lead to an infection. Or an ulcer that can form due to the excess swelling and fluid.
- Topical steroid cream: Hydrocortisone cream can be purchased over the counter. It is a steroid cream that helps to reduce skin inflammation.
- Anti-itch creams: Other anti-itching creams, like Calamine lotion, can be used to help with the itching.
- Antihistamines: This medication helps to reduce the histamine, thereby reducing the itch.
- Compression stockings: Wearing compression stockings can also help improve circulation in the legs.
- Keep moving: Light exercise, such as walking, keeps your legs’ circulation moving.
Bauerfeind has a variety of non-surgical options to relieve the symptoms of varicose veins.
Although the above will provide relief, unfortunately, these will only treat the symptoms. To completely eliminate varicose eczema, the damaged veins will need to be treated or removed.
Seek expert advice
The doctors at The Vein Institute specialise in varicose vein treatment. We offer patients a comprehensive program using non-surgical laser treatment techniques. You can learn more in our Definitive Guide to Varicose Vein Treatment.
The benefits of non-surgical varicose vein treatment are:
- Walk-in walk-out treatment
- 98% success rate
- Extremely effective
- Can be performed at a clinic (no hospitalisation)
- No general anaesthetic
- Medicare rebates apply
- No downtime or time away from work
Call us at 13 VEINS (that’s 13 83467), or fill out our booking request form.




