Chronic venous insufficiency (known as CVI) is a condition that affects the veins in your legs. When it occurs, blood doesn’t flow back to the heart properly, causing it to pool and leading to varicose veins. CVI can result in a range of symptoms, some as mild as itchiness or swelling in the legs, while others can be more severe, including ulcers and intermittent pain.
Roughly 40 per cent of the population suffers from Chronic Venous Insufficiency, so how do you know if you’re vulnerable? Below are the top risk factors for chronic venous insufficiency.
What is Chronic Venous Insufficiency?
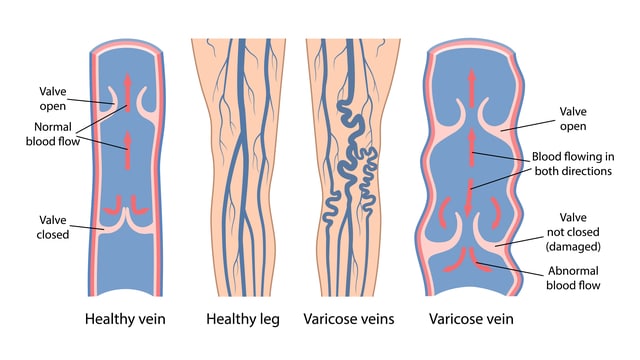
Your arteries carry oxygen-rich blood away from your heart, and veins return it for oxygenation. We have deep veins surrounded by muscles that help propel the blood forward. Then we have more superficial veins situated in the skin’s fatty layer. These types of veins are not influenced by muscles, but they are part of a complex venous network. Both types of veins have flaps of tissue called “vein valves.”
As the blood travels along the veins to the heart, the vein valves ensure it flows in one direction only. Think of it as a swinging door that pushes the blood inside but doesn’t allow it to flow in reverse. If the effects of gravity or muscle contractions cause the blood to pool or try to back up, the vein valve closes automatically, preventing the blood from flowing backward. When the veins overstrain, the valves that pump the blood in the right direction can become overstrained, and the vein walls become stretched and weakened, leading to a backflow of blood that can start to leak into the surrounding tissue if left untreated.
This is most often due to blood clots forming in the veins from a build-up of plaque, or in less common cases, from damage direct to the vein (bone fractures, severe injuries, etc.)
What Causes Chronic Venous Insufficiency?
While many different circumstances can have a small impact on your veins, certain things can increase the risk of chronic venous insufficiency. These include:
- Age
- Genetic predisposition
- Excess weight
- Smoking
- Hormones
- Poor lifestyle
As with varicose veins, CVI often results from unhealthy eating habits, a sedentary lifestyle, and uncontrollable factors like ageing veins and genetics.
Symptoms of CVI and faulty vein valves
It’s important to seek specialist advice if you have the following symptoms:
- Swelling in your lower legs and/or ankles
- Pain or fatigue when walking or standing
- Tight, itchy or uncomfortable feeling in the calves
- Persistent leg ulcers that don’t go away on their own
- The skin on your lower legs looks discoloured or ‘leathery’
How to manage chronic venous insufficiency
CVI itself doesn’t have a simple cure, but with some lifestyle changes and simple efforts, you can reduce your risk of it worsening or developing in the first place and manage any current symptoms.
- Start a regular exercise routine. At least 20 minutes of walking per day helps.
- Wearing medical-grade compression stockings compensates for poor blood flow.
- Cut down on trans and saturated fats and processed sugars, and eat plant-based food like leafy greens, fruit and vegetables.
- If you smoke, speak to your GP to get help to quit for good.
- Check your family history and understand your risk to see how you can stay ahead of it.
- In cases where varicose veins have developed, see a vein specialist to look at treatment options.
In summary
Chronic Venous Insufficiency is often the precursor to varicose veins, so it’s important to stay on top of the condition. Recognising the symptoms, making a few lifestyle changes, and seeking specialist advice are important to slow the condition’s progression.
Seek expert advice
The doctors at The Vein Institute specialise in varicose vein treatment. We offer patients a comprehensive program using non-surgical laser treatment techniques. To book a consultation and discuss our treatment program, call 0420 102 637 or enquire via the Contact Us page.