Varicose veins are a venous disorder. And as we have veins all over our bodies, there are a few places varicose veins can pop up, some more common than others.
Varicose veins often appear in the legs

Close up of varicose leg veins around the back of the knee
Varicose veins typically develop around the lower extremities, like your thighs, calves, ankles, and feet. Additionally, they’ll often appear on the left side, which specialists speculate may be due to your left side having more veins than the right. Your leg veins constantly pull your blood to your heart against gravity, which strains the vein walls and valves. Over time, the valves may malfunction, and your blood will start to pool (reflux), leaving the walls to balloon outward and your leg veins to turn varicose.
A good way to protect your leg veins is to:
- Avoid standing and sitting for hours on end
- If you have to stand or sit for long periods, take breaks to walk around or stretch
- Get compression stockings to help regulate your circulation
- Elevate your legs for a few minutes a day
- And most importantly, exercise
Arms

Close up of a man in a red shirt flexing his arm muscle
Arm veins can turn varicose for similar reasons to leg veins. Genetics, ageing, and hormones can all contribute to your vein walls weakening and your blood refluxing. But, varicose arm veins are much rarer because the threat of gravity is reduced.
Also similarly to leg veins, you can reduce your risk of developing them through exercise and elevation.
Oesophagus
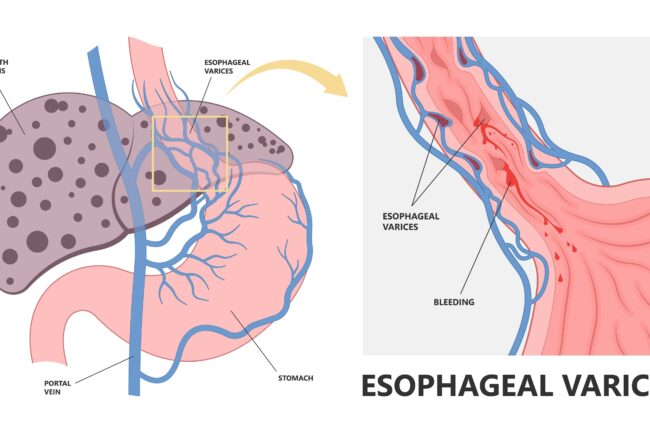
Illustration of oesophageal varices. On the left is the liver undergoing Cirrhosis, and on the right are the bleeding varicose veins that can be caused by it.
A more surprising place for varicose veins to pop up is oesophagus. Most often, oesophageal varices develop due to blocked or impacted blood flow in your portal vein, which is responsible for getting blood from your liver to your heart.
As the vein backs up and the blood has trouble getting from point a to point b, your body will try to reroute it through surrounding smaller veins. But as these veins can’t deal with the increase in blood flow, they swell. And may sometimes rupture or bleed.
So, to reduce your risks, protect your liver by eating a healthy diet and keeping your alcohol intake to a minimum.
Genitals

Illustration of two testes. The one on the left has healthy veins, while the one on the right has a varicocele (varicose vein)
There are two types of varicose veins that develop around the genitals:
- Vulvar varicose veins, which appear around the vulva
- And varicoceles, which appear in the groin
Vulvar varicose veins (also known as a vulvar varicosity) are typically caused by pregnancy. Your progesterone levels rise and your blood supply doubles, leading to lax vein walls and increased blood pressure. On top of that, the added weight of your baby also increases pressure in your pelvic veins. The good news is, in most cases, vulvar varicose veins aren’t dangerous and will typically go away on their own. And there are some steps you can take to manage the symptoms and prevent further damage to your veins.
These include:
- Pelvic floor exercises
- Taking breaks from sitting or standing to walk around or stretch
- Wearing full compression stockings or supportive underwear
- Avoid straining when using the bathroom
Varicoceles, meanwhile, predominantly affect men between the ages of 15-25 and are thought to be caused by the rapid changes brought on by puberty. As you go through growth spurts, so do your testes, and to accommodate the change, your blood supply increases. This results in increased venous pressure and may cause reflux.
Now, varicose veins in the scrotum aren’t dangerous. But in some cases, they can lead to lower testosterone levels and even infertility. So, keep your veins in good health by drinking plenty of water and exercising regularly. We also recommend seeking specialist care if you feel pain, see a worm-like mass, or shrinkage in one or both of your testicles. Note: in ~80% of cases, it’s the left testicle that’s affected.
Pelvis

Close up of woman laying on her side on her couch, clutching her pelvis in pain
Varicose veins may also appear in the ovarian veins, a condition known as Pelvic Congestion Syndrome. These veins may be attached to varicose veins in the vulva and even your legs, and like vulvar varicose veins are usually brought on by pregnancy.
The symptoms may include chronic pain that varies between a dull ache and sharp pain, usually on the left side of your pelvis. This pain commonly starts during pregnancy and worsens during sexual activity, menstruation, walking, and sitting or standing for long periods. You may also experience back pain, fatigue, and itching or swelling around your pelvis.
To help you avoid it and manage symptoms, get plenty of exercise, drink plenty of water, and keep your pelvic floor in good shape.
Rectum

Young businesswoman with hemorrhoids holding her hip to relieve pain
The rectum is another area where varicose veins can pop up. Also known as haemorrhoids, these varicosities may develop due to the pressures of pregnancy. They may also form due to constipation, when you have to strain to have a bowel movement.
So, along with maintaining good vein health, you should also include plenty of fruits, veggies, and fibre in your diet to help things move along.
When to see a specialist
Varicose veins aren’t a dangerous condition. In some cases, you might not even know you have them. But, as they can be unsightly, painful, and may lead to dangerous conditions like deep vein thrombosis, you should see a specialist if you suspect you have them. And especially if they’re bothering you.
Remember, while you can manage your varicose vein symptoms on your own, medical intervention is the only way to treat varicose veins. Luckily, treatments have come a long way. Vein specialists can use embolization to treat varicose veins in more sensitive areas like the scrotum and vulva.
And we at The Vein Institute specifically can treat varicose veins in your legs via minimally invasive procedures like medical superglue, sclerotherapy, EVLA, RFA, Flebogrif or ClariVein.

