May-Thurner syndrome is a condition that involves your right iliac artery, which carries blood to your right leg. And the left iliac vein, which returns blood from your left leg toward your heart. Other names for this disorder are iliac vein compression syndrome and Cockett’s syndrome. It is important for you to understand what causes May-Thurner Syndrome. Because although it is not always a medical concern, it can be linked to the development of Deep Vein Thrombosis.
What is May-Thurner Syndrome?
Patients who suffer from May-Thurner syndrome have an anatomical irregularity that causes the right iliac artery to squeeze the left iliac vein as they cross each other in the pelvis. As a result, the increased pressure constricts the flow of blood through the left iliac vein, much like stepping on a garden hose.
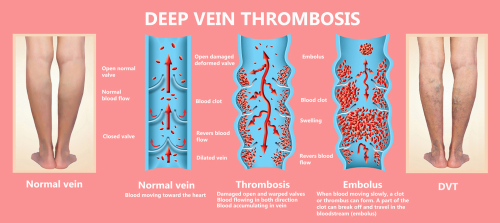
May-Thurner syndrome can be particularly problematic for some patients. Not only does it restrict blood flow, but it can also increase your chances of developing a blood clot called DVT or deep vein thrombosis in your left leg. DVT is dangerous because it can break off and travel to your lungs, causing a life-threatening condition known as a pulmonary embolism.
No genetic link with May-Thurner Syndrome
Up to 20% of the population may be predisposed to May-Thurner syndrome. If you fall into this demographic, you have the anatomical irregularity where the right iliac artery overlies and can potentially compress your left iliac vein. Even so, the occurrence of May-Thurner syndrome is random and does not appear to be inherited from your relatives.
What causes May-Thurner Syndrome?
You should note that blood vessel crossover in the body is common and perfectly normal. Problems only arise when they are positioned in a way that causes the right iliac artery to press the left iliac vein against the spine. You’re at greater risk of developing May-Thurner syndrome if you:
- Are female
- Have scoliosis
- Had one or more pregnancies
- Take oral contraception pills
- Have a blood clotting disorder
- Sit for long periods of time
Symptoms
Other than pain and swelling in your left leg, May-Thurner’s syndrome doesn’t always present any warning signs. In fact, most patients don’t even know that they have this condition until they develop a DVT. With DVT, however, there are clearly identifiable symptoms, including:
- Pain and intense cramping in the left leg
- Heaviness, tenderness, or throbbing
- Veins that look enlarged or dilated
- Skin that’s warm to the touch
- Swelling and inflammation
- Changes in skin colour
- Diagnosis and treatment
First, your physician will perform a physical exam to assess and detect any symptoms and possible complications of DVT. Next, they will “look” inside your circulatory system using various imaging devices, including ultrasound.
If they don’t detect blood clots in your leg and your May-Thurner’s syndrome is diagnosed as mild, you can manage it by following a healthy lifestyle and wearing compression stockings. These are tight garments that typically extend from your toes to the knee. They put gradual pressure on your lower legs, helping to ease swelling and promote improved blood flow.
You may have other veins disorders
Your doctor may determine that the cause of your leg swelling and discomfort is actually a varicose vein. This is a vein condition where faulty vein valves result in blood flowing backwards and pooling in the veins, causing them to become twisted and dilated.
Phlebologists or other vein specialists normally treat varicose veins. Based on the severity of the disease, they may recommend a number of treatment options, including Sclerotherapy, Endovenous Laser Therapy (EVLA) and Radiofrequency Ablation (RFA), ClariVein, or VenaSeal vein glue.
Seek expert advice
The doctors at The Vein Institute specialise in varicose vein treatment. We offer patients a comprehensive program using non-surgical laser treatment techniques. You can learn more in our Definitive Guide to Varicose Vein Treatment.
The benefits of non-surgical varicose vein treatment are:
- Walk-in walk-out treatment
- 98% success rate
- Extremely effective
- Can be performed at a clinic (no hospitalisation)
- No general anaesthetic
- Medicare rebates apply
- No downtime or time away from work
To book a consultation and discuss our treatment program, call 0420 102 637. Or, make an enquiry via the Contact Us page.