Why do my veins hurt?
Do I need varicose vein treatment?
How to get rid of spider veins
Veins and their various conditions can be a bit of a mystery to non-specialists. So, it’s not surprising that many of our patients ask questions like these. To help you understand your venous system a little better, we’re answering some of your commonly asked vein questions below.
1. Why do I have bulging veins in my feet?
The veins in your feet are in a stressful position. They have to work hard against gravity to push deoxygenated blood back to the heart. Over the course of a day (especially if you’ve been on your feet or sitting with your feet on the floor), some of the blood can start building up in the foot veins, causing them to bulge.
Typically, some protrusion is perfectly normal, especially in the evening or after strenuous exercise. However, if you start noticing your foot veins growing darker and more twisted or experiencing pain, itching, or burning sensations, you should see a specialist.
In the meantime, you can take some steps to improve your circulation, which may help improve the vein’s appearance and keep surrounding veins happy and healthy.
Learn more: How to Keep Your Circulatory System Healthy
2. Why do my veins hurt?
There are a few venous disorders that cause vein pain. These include:
- Varicose veins. These are large, bulging, twisted veins that can irritate surrounding tissue, causing burning sensations, muscle cramps, and a dull ache that gets worse at night.
- Chronic venous insufficiency. Usually the precursor of varicose veins, this condition stems from the little valves in your veins not closing properly, causing blood to pool. As with varicose veins, you may experience some swelling, itching, cramping, fatigue, and a dull ache. The distinction is that CVI doesn’t include vein bulging (yet).
- Deep Vein Thrombosis. DVT is when a blood clot forms in one of your deep veins. You may experience pain, swelling, and redness in the affected area.
- Superficial thrombophlebitis. This condition is essentially DVT that occurs in the surface veins instead of the deep ones.
- Cellulitis. It’s an infection of the tissues below the skin surface, which can spread to surface veins. It can occur from bacteria breaching the skin through a cut and is more likely to happen if you have a condition that makes it harder for wounds to heal (like diabetes). You may experience pain, tenderness over the affected area, and swelling. You may also get a fever.
Vein pain may also occur or worsen after long hours of standing. As you can see, it can be a bit difficult to distinguish between some of these conditions yourself. That’s why if you start experiencing these symptoms, you should see a specialist for ultrasound imaging and a proper diagnosis. That’s the only way we can determine the best course of action for you.
3. Why are veins blue
The colours we see depend on the different wavelengths of light that hit them and bounce back to our eyes. Veins appear blue, green, and sometimes purple because cooler colours have shorter wavelengths. While red light will penetrate the skin, greens and blues will bounce back to our eyes.
4. How to get rid of spider veins
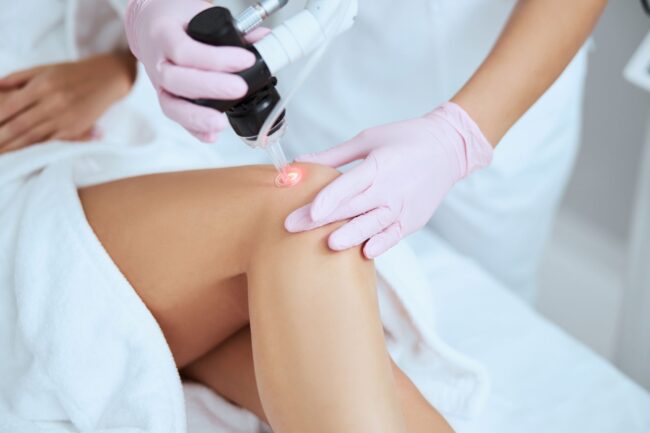
Doctor using a topical laser treatment to treat a patient’s spider veins
As with varicose veins, the only way to get rid of spider veins is through medical treatment. Creams, herbal supplements, and apple cider vinegar will not work, regardless of what some health blogs tell you.
Currently, medical treatments for spider veins include:
- Sclerotherapy, in which your doctor will inject tiny amounts of an irritant into the vein, sealing it off and letting your body absorb it over time. Generally, you’ll need 2-3 rounds of sclerotherapy for good results.
- Topical laser treatment, in which your doctor will use a specialised laser to deliver target bursts of light to the problem vein, causing it to fade over time. As with sclerotherapy, you’ll need 2-3 rounds for good results.
As spider veins often come connected to varicose veins, we’ll need to treat the varicose vein first.
Please note, however, spider veins are a touch more finicky to treat than varicose veins.
Learn more: Treating Spider Veins vs Treating Varicose Veins
5. Why are the veins on my face so visible?
Vein visibility depends on a few things:
- Skin thickness: the thinner your skin, the more visible your veins.
- Skin pigmentation: generally, veins stand out more when contrasted against lighter skin tones
- Blood pressure levels: hanging upside down, strenuous exercise and certain foods can raise your blood pressure, causing your veins to expand a little and stand out more.
- Environment: cold weather shrinks your veins but hot weather dilates your veins, and prolonged sun exposure damages the collagen in your skin, making your veins more visible
- Genetics: visible face veins can also just be inherited.
6. How do I know if I have varicose veins?
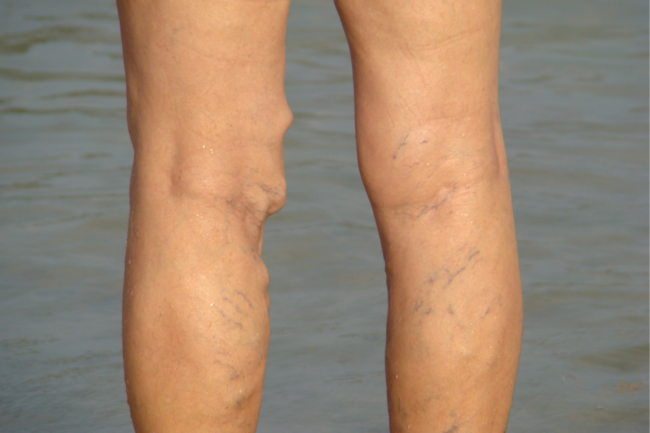
Person with bulging varicose vein standing at the beach
“Why do my veins hurt?” You might be getting a varicose vein.
Typically, you can identify varicose veins pretty easily. They’re large, bulging, twisted veins that often appear dark blue, green, or fleshy. They also come with uncomfortable symptoms like itching, burning, pain, limb fatigue, and swelling.
However, varicose veins don’t always pop up above the skin’s surface or cause symptoms. So, if you’re worried or unsure of your vein condition, see a specialist for a thorough examination and a diagnosis.
7. What are superficial and deep veins?
Superficial veins are smaller veins close to the skin’s surface. They move blood out of skin cells and other tissues for waste removal in the kidneys and oxygenation in the lungs. Deep veins, on the other hand, are large veins deep under the skin. These have a surrounding muscle layer to help pump all the blood collected from surface veins to the heart.
8. Do I need treatment for varicose veins?
To get rid of your varicose veins, yes. You will need treatment. There are some people who opt not to get medical treatment, whether that’s because they’re afraid to get vascular surgery or aren’t experiencing any ill effects from the condition.
But we can’t emphasize enough that varicose veins can progress and worsen over time, potentially leading to dangerous conditions like ulcers and often irreversible skin damage.
We also can’t emphasize enough that vascular surgery is NOT your only option. Recent advancements in medical technology allow us to perform minimally invasive, walk-in, walk-out treatments that are considered safer and often just as effective as surgery. These include:
- Endovenous Laser Ablation (EVLA). During this treatment, we insert a thin laser wire into your vein to heat it up.
- Radiofrequency Ablation (AKA RFA). This treatment is very similar to EVLA, the key difference being we use short radiofrequency bursts to heat up the vein instead of a laser.
- Medical Superglue (AKA VenaSeal). Here, we use either a tiny catheter or a syringe to inject cyanoacrylate glue into the problem vein and apply gentle pressure to glue it shut.
- Sclerotherapy. Similar to the spider vein treatment, we’ll inject sclerosant into the problem vein to agitate it.
- ClariVein. This treatment is essentially a more robust version of sclerotherapy. Instead of a syringe, we’ll use the specialised ClariVein Catheter to inject sclerosant into the problem vein. The catheter’s rotating tip allows us to cover more ground, letting us use sclerosant for medium-sized varicose veins instead of only small ones.
9. Can I tattoo over my varicose veins?
It’s not a good idea to tattoo over your varicose veins. These veins are oversized, bulging, and prone to bursting. So, the pressure of a tattoo needle can cause pain or even rupture the vein.
10. Will varicose veins go away if I lose weight?
Too much excess weight can strain the veins and contribute to a vein disorder. However, if you already have varicose veins, the only thing that can make them ‘go away’ is treatment. Living a healthy lifestyle pre and post-op is beneficial as it can reduce the risk of new varicose veins forming.
Learn more: Non-Surgical Varicose Vein Treatments and Technologies Used
To start your varicose vein treatment journey, call us on 0420 102 637 or request an appointment online.
