Varicose veins often pop up in the legs. But their underlying cause (venous insufficiency) can also affect your feet and ankles. As the condition is extremely common (affecting approximately 500,000 Australians), it’s important to know its causes, symptoms, and management and treatment options.
What causes varicose veins in the foot?
Varicose veins generally occur when the tiny valves in your veins become damaged or weakened (a condition known as Chronic Venous Insufficiency, or CVI). Varicose veins in the feet don’t often turn varicose on their own. Instead, they typically form due to CVI or varicose veins in the legs. Because your foot veins can no longer rely on your leg veins to move blood out, blood pools, pressure builds, and their walls stretch out and turn varicose. The exact cause is unknown, but you’ll be more at risk depending on your:
The bottom line is that varicose veins happen when your blood doesn’t circulate properly around your body (whether due to vein damage or strain). This abnormal circulation leads to blood pooling in your veins, eventually turning them varicose.
As you can imagine, your legs, feet and ankle veins undergo the most pressure from weight and gravity. So, you’re most at risk of developing varicose veins there.
What are the symptoms of varicose veins in ankles and feet?
- Numbness in your feet
- Pain around your feet and ankles
- Throbbing, itching and burning in feet and ankles
- Redness, swelling, tenderness around feet and ankles
- Ulceration or broken skin around feet and ankles
- Restless or heavy legs and frequent cramping
How is foot and ankle swelling linked to varicose veins?
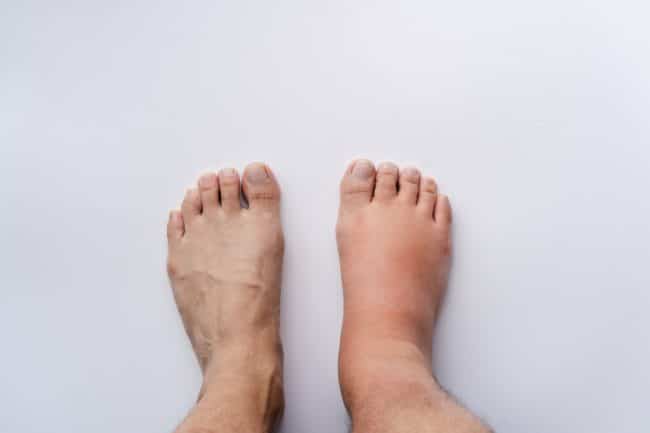
When the veins in your feet and ankles turn varicose, their walls are too weak to keep blood flowing. As a result, fluid builds up in the surrounding tissue, causing swelling like in the picture above.
While varicose veins don’t directly cause this swelling, underlying vein-aggravating issues like oedema, lymphedema, and phlebolymphedema might.
If you find that the swelling in your legs is chronic and you have varicose veins, it’s worth talking to your doctor about as they can treat it.
What happens if you don’t treat varicose veins?
It depends on your situation. If you’re not experiencing discomfort (either of the aesthetic or physical variety), you might not need medical intervention. You could instead opt for home remedies such as low-impact exercise, compression, and elevation.
However, those bluish veins around the feet and ankles can lead to more serious health conditions. Therefore, no matter your comfort level, you should still speak with your doctor and receive a proper diagnosis and treatment plan.
If you leave problematic varicose veins too long without intervention, it can lead to:
- Blood clots in the legs and other parts of the body
- Venous eczema
- Discoloured or ulcerated skin
- Swelling and hardening of the skin on your feet, ankles and lower legs
What are the treatment options?
Above all, advanced cases of venous insufficiency may require medical intervention. Fortunately, we offer some excellent non-surgical approaches to treating varicose veins:
- Endovenous Laser Ablation (EVLA) – laser energy to close off the abnormal veins and minimise their appearance.
- Radiofrequency Ablation (RFA) – radiofrequency energy directed through a thin tube (called a catheter) to close off the blood flow.
- Medical Superglue – physically glues and seals defective veins.
- Sclerotherapy – involves injecting a safe pharmaceutical solution directly into the affected vein to irritate the lining of the blood vessel, causing it to collapse.
- ClariVein: This is a specialised catheter with a rotating tip. We use it to inject sclerosant deeper into the vein to seal it off.
How are varicose veins in the feet treated?
Vein specialists don’t usually treat varicose veins in the feet initially. Instead, they’ll treat the leg veins they’re attached to first and then address the foot veins, owing to the sensitive region they’re in. Foot veins are close to deep veins and other sensitive structures, meaning the risk of treating them directly is higher. And if the foot veins are treated in isolation, there’s a chance that any underlying venous insufficiency in the leg will turn them varicose again.
When your vein doctor seals a leg vein, your blood will stop flowing through it from the foot vein. Your body will automatically reroute blood flow to nearby healthy veins and absorb the varicose one along with all the veins relying on it to transport blood to the heart.
And don’t worry. You don’t need those veins for good circulation. Superficial veins are usually the ones to turn varicose, and they’re collectively only responsible for about 10% of your blood flow.
See where else varicose veins can form: Where Can Varicose Veins Pop Up
Seek specialist advice
Do you think you have varicose veins in your feet or ankles? Give us a call on 0420 102 637 or enquire via the Contact Us page. We’ll be happy to consult you on management and treatment options.